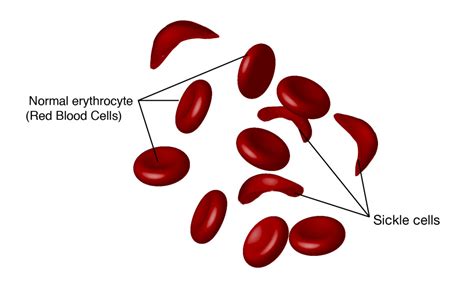
Navigating health insurance for individuals with sickle cell disease (SCD) can seem like an overwhelming and complex task. The unique challenges posed by SCD—a genetic condition affecting red blood cells—require a nuanced understanding of health insurance policies and coverage options. This article aims to simplify this labyrinth for both patients and caregivers by presenting a clear, expert perspective grounded in practical insights and evidence-based information.
Understanding Health Insurance for Sickle Cell Disease
Sickle cell disease necessitates regular medical care and often results in high out-of-pocket costs. This can be especially challenging for those with limited financial resources. Understanding the specifics of health insurance coverage for SCD is crucial. Policies vary widely in what they cover, and being well-informed can make a significant difference in managing the disease’s medical and financial burdens.
Key Insights
- Primary insight with practical relevance: Patients with SCD should review their health insurance policies carefully, focusing on the coverage for specialty care, medications, and treatments.
- Technical consideration with clear application: Pay particular attention to co-payments, deductibles, and out-of-pocket maximums, as these can have a direct impact on financial planning for ongoing treatments.
- Actionable recommendation: Seek assistance from a patient advocate or healthcare navigator to better understand and optimize your health insurance benefits.
Coverage for Specialty Care
Individuals with sickle cell disease often require visits to specialists such as hematologists or pain management clinics. Health insurance plans typically cover these visits, but the extent of this coverage can vary. Some plans may impose restrictions, such as prior authorization requirements for specialist appointments. An example would be a plan that requires pre-approval for visits to a pain management specialist but allows full coverage once approval is granted.
Medication and Treatment Coverage
The management of sickle cell disease frequently includes prescription medications and sometimes advanced treatments like stem cell transplants. The availability and coverage of these treatments can differ significantly among health plans. For instance, hydroxyurea—a common medication for SCD—may be fully covered by one plan but have substantial co-payments under another. It is crucial to understand not just whether these medications are covered, but also the level of coverage and any associated out-of-pocket costs.
Can my health insurance plan change after I’ve been diagnosed with sickle cell disease?
No, under the Affordable Care Act (ACA), health insurance companies cannot change your coverage or deny you based on a pre-existing condition such as sickle cell disease. This protects individuals with chronic illnesses from being penalized or left without coverage.
What should I do if my health insurance plan doesn’t cover a necessary treatment?
If your current plan does not cover a necessary treatment, explore options for appealing the decision or consider enrolling in a different plan that offers more comprehensive coverage. Additionally, patient advocacy groups can offer support and may be able to connect you with resources to help pay for treatments not covered by your insurance.
In conclusion, managing sickle cell disease with the help of health insurance requires thorough understanding and active engagement with your policy. By staying informed about what your plan covers and seeking out additional support when necessary, you can better manage both the medical and financial aspects of living with this chronic condition.